 
Once these forms are reviewed a letter is sent to the member and provider by mail to confirm or decline the service request. The forms are available on the Forms page or by calling the BCBSIL Behavioral Health Unit. Refer to the Provider Tools section for more information, including an Availity Authorizations User Guide .Īs part of the initial prior authorization process, the provider must complete and submit the appropriate ABA form to confirm the requested information. Once the completed forms are reviewed a letter is sent to the member and provider by mail to confirm or decline the service request.Īdditionally, providers may use the Availity Authorizations tool to submit electronic prior authorization requests for inpatient admissions and select outpatient services that require prior authorization through BCBSIL. Prior authorization for these services requires completion of a form or forms, as listed on the Forms page. Intensive Outpatient Programs (IOPs), Outpatient ECT or rTMS Outpatient – Members should call the behavioral health number on their BCBSIL ID card. For these outpatient services, prior authorization requires completion of a form located on the Forms page. Inpatient and Alternative Levels of Care – Members should call the appropriate number on the their BCBSIL ID card. BCBSIL will comply with all federal and state confidentiality regulations before releasing any information about the member. All services must be medically necessary. Behavioral health providers or a member’s family member may request prior authorization on behalf of the member. Members are responsible for requesting prior authorization when prior authorization is required.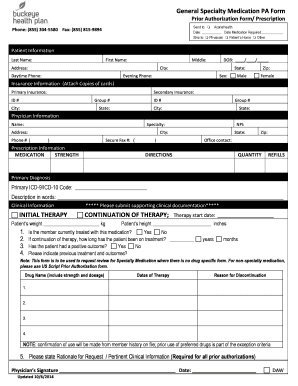  
What’s the process for submitting prior authorization requests? This prior authorization requirement only applies for members who have Behavioral Health Outpatient Management as part of their behavioral health benefit plan through BCBSIL.Īdditionally, Federal Employee Program ® (FEP ®) members must request prior authorization for ABA services but are not required to request prior authorization for PHP or any other outpatient behavioral health services.įor prior authorization requirements summaries and procedure code lists for Medicare Advantage PPO and Illinois Medicaid members, refer to the Support Materials (Government Programs) page. To determine benefit coverage prior to the service and to determine if prior authorization for intensive outpatient services may be required by a specific employer group, members may call the prior authorization MH/SA number listed on their ID card or the BCBSIL Behavioral Health Call Center at 80. Psychological and Neuropsychological Testing, in some cases (BCBSIL will notify the provider if prior authorization is required for these testing services).Repetitive Transcranial Magnetic Stimulation (rTMS).Outpatient Electroconvulsive Therapy (ECT).This requirement applies only for members who have outpatient management as part of their behavioral health benefit plan through BCBSIL. These intensive outpatient services require prior authorization to confirm that the services are medically necessary, clinically appropriate and contribute to the successful outcome of treatment: However, notification is encouraged after admission to the facility. Out-of-network unplanned or emergency hospital admissions and post-stabilization services do not require notification. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
